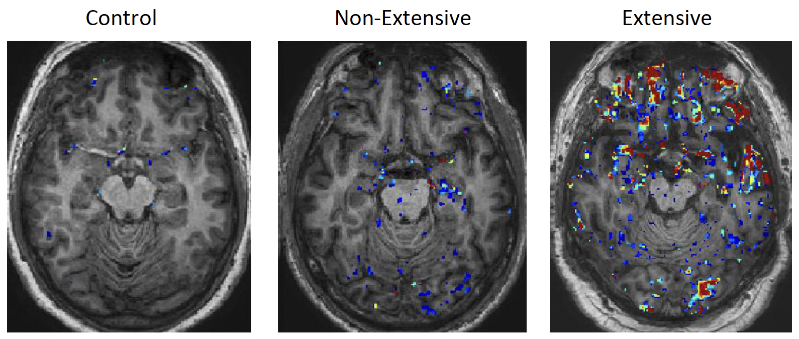
Factors Not Considered in the Study of Drug-Resistant Epilepsy: Drug-Resistant Epilepsy: Assessment of Neuroinflammation
March 15, 2022
Abstract found on Wiley Online Library
ABSTRACT
More than one-third of people with epilepsy develop drug-resistant epilepsy (DRE). Different hypotheses have been proposed to explain the origin of DRE. Accumulating evidence suggests the contribution of neuroinflammation, modifications in the integrity of the blood-brain barrier (BBB), and altered immune responses in the pathophysiology of DRE. The inflammatory response is mainly due to the increase of cytokines and related molecules; these molecules have neuromodulatory effects that contribute to hyperexcitability in neural networks that cause seizure generation. Some patients with DRE display the presence of autoantibodies in the serum and mainly cerebrospinal fluid. These patients are refractory to the different treatments with standard antiseizure medications (ASMs), and they could be responding well to immunomodulatory therapies. This observation emphasizes that the etiopathogenesis of DRE is involved with immunology responses and associated long-term events and chronic inflammation processes. Furthermore, multiple studies have shown that functional polymorphisms as risk factors are involved in inflammation processes. Several relevant polymorphisms could be considered risk factors involved in inflammation-related DRE such as receptor for advanced glycation end products (RAGE) and interleukin 1? (IL-1?). All these evidences sustained the hypothesis that the chronic inflammation process is associated with the DRE. However, the effect of the chronic inflammation process should be investigated in further clinical studies to promote the development of novel therapeutics useful in treatment of DRE.