Seizures are terrifying.
I witnessed a seizure for the first time when my son, Isaiah, was four months old. I held his rigid body in my hands as his eyes fluttered in the back of his head and his legs jerked uncontrollably. That first seizure lasted more than 10 minutes.
It felt like an eternity.
I met my husband Pat on a rugby pitch at Radford University in 1993. He was athletic, confident, and always willing to lend a hand. When he graduated, he enlisted in the Army out of love for his country and a desire to remain active.
Pat was deployed to Iraq with the Arrowhead brigade in June 2006. On July 7, 2007, Pat was on a night mission in a Baghdad neighborhood. After being there for many hours, a soldier and Pat were going downstairs to get water for the soldiers. He was shot from across the street.
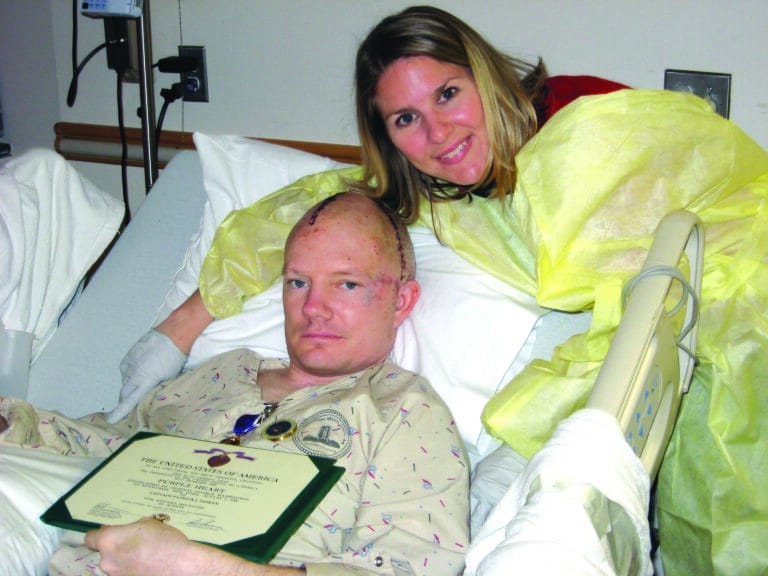
Pat’s traumatic brain injury was grave, and at the field hospital, the medical staff had no choice but to remove half of his skull to allow his brain to swell. Since that frightful day, Pat has worked hard to regain his ability to do things we used to take for granted: use his right arm, walk, talk, write, and read.
However, the biggest stumbling block has been the post-traumatic epilepsy (PTE). I’ve never been more frightened than when Pat experienced his first seizure five months after his injury. I truly thought he was dying. With a brain injury, most of your recovery occurs in the first two years. Pat has had to work extra hard to make gains. Pat is now on two seizure medications. We hope that this combination will do the trick. Pat had his last seizure in 2014.
I often wonder what Pat’s recovery would have been like without PTE. We have been the beneficiaries of best of what humanity has to offer. The support from people we have met and the organizations we are part of have brought us hope in times of struggle. Every year Pat participates in the Army Ten Miler race. We organize with “Pat’s Team” of over 75 runners. The event has provided us with a connection to family, friends and a community otherwise not possible. Pat is also active with CURE Epilepsy. We get a chance to share our story of hope with others in need.