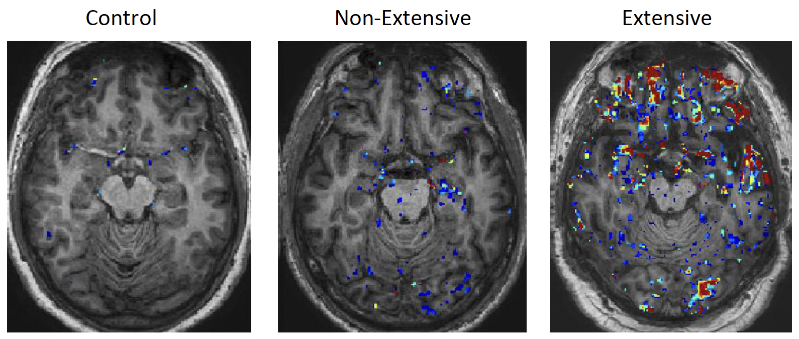
The Common Pathways of Epileptogenesis in Patients With Epilepsy Post-Brain Injury: Findings From a Systematic Review and Meta-Analysis
August 10, 2023
Abstract found on PubMed
Background and objective: Epilepsy may result from various brain injuries, including stroke (ischemic and hemorrhagic), traumatic brain injury, and infections. Identifying shared common biological pathways and biomarkers of the epileptogenic process initiated by the different injuries may lead to novel targets for preventing the development of epilepsy. We systematically reviewed biofluid biomarkers to test their association with the risk of post-brain injury epilepsy.
Methods: We searched articles until January 25, 2022, in MEDLINE, Embase, PsycINFO, Web of Science, and Cochrane. The primary outcome was the difference in mean biomarker levels in patients with and without post-brain injury epilepsy. We used the modified quality score on prognostic studies for risk of bias assessment. We calculated each biomarker’s pooled standardized mean difference (SMD) and 95% confidence intervals (CI). Molecular interaction network and enrichment analyses were conducted in Cytoscape. (PROSPERO CRD42021297110) RESULTS: We included 22 studies with 1499 cases with post-brain injury epilepsy and 7929 controls without post-brain injury epilepsy. Forty-five biomarkers in blood or cerebrospinal fluid (CSF) were investigated with samples collected at disparate time points. Of 22 studies, 21 had a moderate-to-high risk of bias. Most biomarkers (28/45) were investigated in single studies; only nine provided validation data, and studies used variable definitions for early and late-onset seizures. A meta-analysis was possible for 19 biomarkers. Blood glucose levels in four studies were significantly higher in patients with post-stroke epilepsy (PSE) than without PSE (SMD 0.44; CI 0.19 to 0.69). From individual studies, 15 biomarkers in blood and seven in CSF were significantly associated with post-brain injury epilepsy. Enrichment analysis identified that the significant biomarkers (IL6, IL1?) were predominantly inflammation related.
Discussion: We cannot yet recommend using the reported biomarkers for designing anti-epileptogenesis trials or use in the clinical setting because of methodological heterogeneity, bias in the included studies, and insufficient validation studies. Even though our analyses indicate the plausible role of inflammation in epileptogenesis, this is likely not the only mechanism. For example, an individual’s genetic susceptibilities might contribute to his risk of epileptogenesis after brain injury. Rigorously designed biomarker studies with methods acceptable to the regulatory bodies should be conducted.